My TPN Experience and the Steps I Take to Start a TPN Feeding Cycle
First I was given a PICC line, double lumen and was also a power picc meaning it could be used for contrast injection for CT scans. Double lumen was nice as I could stay on TPN while medicine was taken or blood was drawn (with TPN turned off but still attached mind you – too many times was it still running and I’d get frantic calls back telling me my glucose levels were over 700). They could also put me on fluids while TPN was running through the other line. They could have me hooked up to a whole bunch of things at once without one single needle poke, and well, they did.
It worked out pretty well until I got home, where I quickly learned that a PICC line was not for me…

Before figuring out what was going to happen with my PICC line and how long I’d be on TPN, I needed to talk with my doctors. I was informed that I could no longer be fitted for feeding tubes as there is no more space in my small abdomen for placement and they also cause me pain. With this in mind, I will be on TPN indefinitely in some form or another for all or supplemental nutrition for a good portion of my life. If this is the case, PICC lines dangling down from my arm for Ellie to pull on and to stop me from fully using my arm to climb or any other physical activity wasn’t going to cut it. I asked for a portacath.
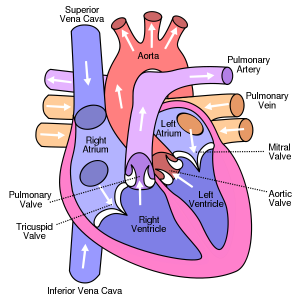
The power port is surgically placed under the skin (usually sutured into the chest wall) by a doctor, surgeon, interventional radiologist, certified nurse with the use of fluoroscopy and xray to make sure the position of the catheter is placed correctly (the tip of the catheter being right above the superior vena cava of the heart).
Mine was placed by an interventional radiologist with sedation and I was sent home later that day to relax. My TV junkie Berner puppy can be seen below. She’s great company when you’re sick, especially if TV is involved. She wouldn’t even look at the camera until commercials. *shakes head*
It was very sore, I won’t lie. Ice packs were my friend. Sadly they would not access my port to start tpn, without orders from my doctor, while I was still sedated, so later that evening it was accessed with a needle to a very freshly closed wound. It has gotten considerably easier though. I am almost one month out. I’ve had setbacks with it. My chest is very sensitive to all the dressings and I have broken out in a horrible horrible painful rash each time it was changed, but I think it is under control now. All I use now is plain Tegaderm with gauze under the wings of the needle to stabilize it.
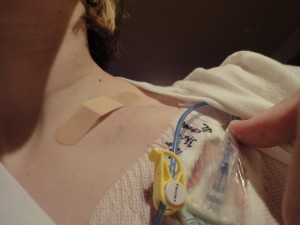
So far TPN seems to be going well. I’m pretty much NPO (nothing by mouth), but will munch on something if I feel like it or take in some juice. I’ve been able to cycle down the time I’m hooked up to TPN to 12 hours at night so that I can be pretty much free during the day. Even without food intake, I get stomach pains – err, abdominal pains and this has stumped all of my doctors. I see a pain specialist at the end of next month. Until then, I’ll make do with what I have available and try to stay out of the ER!
I am not permitted to change the dressing of my port on my own or the line either. I have a home care nurse come to my house every Monday who checks vitals, draws blood (full panel), and changes dressings and needles. I, however, am responsible for starting and finishing my own TPN bags, which, I must say, I have become quite good at!
Also, doctors, parents, friends, and children please remember to always be washing your hands while around other people!
Steps I take to set up my TPN bag and start a feeding session –>
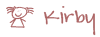
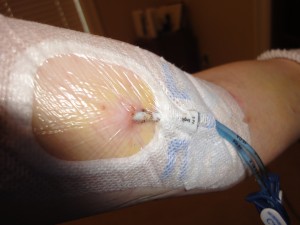
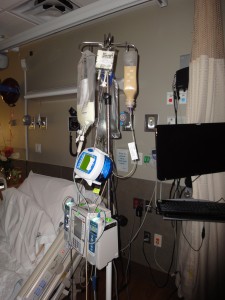









7 Responses
Christina says...
I hope this method is working for you. My husband is newly diagnosised and it has been hell. He is in an out of the hosipital ever week because of constant stomach pain in his uper abdomen. Once the pain out does his pain meds he begins to vomit and then the only way to stop it is with IV medications. Our first GI was for lack of a better term a real idiot. So we see our new GI next week. Was it because you lost so much weight the doctors decided TPN was for you. Is your pain managed more now that you are on TPN? Thank you for sharing!
Kirby says...
While very late in response, TPN was not the first thing they did to counteract my weightloss and worsening malnutrition. I was first given an NJ tube for 6 excruciating months. After that I was given a normal jejunostomy tube. Did well with that, though gained little weight, until they tried to place a button on my suggestion. It all went horribly wrong and I ended up with a surgically placed jejunostomy during an open emergency exploratory surgery. It was this tube that caused scar tissue and chronic pain. My intestines slowed down (CIP) and occasionally stop all together (paralytic ileus). It just became too much and the tube feeding was working against me instead of for me. I was put on TPN a year and a half ago and am still on it now. It has done wonderful things for my weight. And the pain I had from force feeding through the jejunostomy was gone. I still suffer chronic pain due to the scar tissue and whatever they messed up when I was in for that emergency surgery. I am happy with the TPN but worry what might happen if it starts to fail me as well. I really have nothing else to fall back on 🙁
Wendy says...
I happened to stumble upon your story from doing a google search of “living permanently on TPN”. My 52 year old mother has been in the hospital for the last 4 months. They have thrown around the word “gastroparesis”, but she has never officially been diagnosed with this.
Prior to her hospitalization in March, she had been throwing up for well over a year. Sometimes she could eat, and it may be 2-3 days before she vomited, but she always ended up vomiting. In the last few months before her hospitalization, she was vomiting 3-4 times daily.
Within the first few days of her hospital stay, they inserted an NG Tube and drained thousands of CC’s of bile that had accumulated in her stomach. The doctor said her stomach was hugely stretched out from this build up of bile.
However, over the last 4 months she has seen no real improvement. They did an exploratory surgery of her stomach, and ended up removing many bands of scar tissue caused from prior surgeries. (My mother is also in end stage renal disease, and had previously been on peritoneal dialysis at home, which required them to insert a catheter into her abdomen) The surgeon told us, that by removing the bands of scar tissue in her stomach, she may see an improvement and be able to eat and digest her food, but it could take months.
Due to her being severely malnourished by this point, they did another surgery to insert a feed tube. Now I have heard the nurses refer to this a “G” tube, but also a “J” tube, so at this point I am still confused as to what type of feeding tube she actually has.
However, my mother has been unable to tolerate the tube feedings. These also make her sick and cause her to have severe diarrhea. So she keeps ending up back on TPN.
Over the last months they keep trying to see if she will start to tolerate eating food….but it always results in her throwing up, (or having severe pressure/bloated feeling until she throws up). She is still unable to tolerate the feeding tube. Now the doctors are starting to discuss sending my mother home with TPN but she would have to be NPO at all for her insurance to agree to pay for it.
Due to my mother’s other health conditions and the poor health she is now in due to laying in a hospital bed for the last 4 months, she does not feel like she wants to live on TPN with NPO for the rest of her life.
Do you feel like you still maintain a good quality of life living on TPN?
Kirby says...
As to the feeding tube – if she has gastroparesis, they should not and hopefully have not inserted a g-tube (gastric feeding tube) for feeding as the stomach is unable to work. A g-tube used for feeding is only used for those who cannot eat orally, probably due to problems in their esophagus or whatnot, but their stomach still works fine. Usually those with a g-tube used for feeding often use their own mixture of food that is blenderized and bolused or pushed through with a syringe, at mealtime (3 times a day like anyone would if they were eating normally). A j-tube is what I had placed for feeding and you use a special formula that is pumped into the tube (with a special pump) for usually around 12 hours or up to 24 hours (at a slower rate). A g-tube can be placed in those with gastroparesis but is only used to drain the stomach of bile build-up, gas or food that is causing severe abdominal extension or pain. But nothing is ever put into the stomach. Hopefully that will help you know if it is a g-tube or a j-tube and if they are incorrectly feeding into the stomach when she is suspected of having gastroparesis, you can correct them. That may be why she is not tolerating the feeding tube as well.
As for TPN – I live a relatively normal life. There are risks of infection because TPN is delivered via a central line (a PICC, portacath or Hickman), but if proper sterile techniques are taken by everyone, the risk of infection should be lowered. I did well on tube feeding for a year or so, despite not gaining any weight, but for whatever reason, stopped tolerating the tube feeding and had to be placed on TPN and went home on it after a few weeks in the hospital. I have to say, it saved my life. My nutrition is now perfect and my weight stable. Aside from having to carry around a backpack with my TPN in it (it has simply taken the place of a purse with an added bonus of storing more things such as my iPad), I am not limited in activity. When nutrition is restored through TPN, after a few months you do not feel hunger nor have much of an appetite. It may take awhile to reduce cravings for things your body clearly does not need and would most definitely cause more problems anyway, but you do get used to it. If you have any other questions, don’t hesitate to ask. I hope your mother starts feeling better soon. She and your whole family are in my thoughts.
Wendy says...
Thanks for the info!! What you said makes so much sense about my mother’s different types of tubes. She must have a J-tube for feeding, as they put things like Nephro and Jevity into that using a Kangaroo Joey Pump. When I hear them speak of a “G-Tube” they must be referring to the tube that is draining her stomach, because I do know she has one. The bag to it is always hanging off her hospital bed…and besides vomiting that is the only thing that gives her much relief. That makes things much clearer for me!!
Right now she is having a problem with a lot of drainage coming out around one of her tube sights. They said it is stomach acid.
Though she is hooked up to TPN right now, they are also letting her eat as tolerated…which seems crazy to me because it always results in her vomiting up so much bile!! But I guess they keep hoping her stomach with miraculously start working again! And I guess my mother keeps eating because, as she says, she is “freaking hungry!!”
I am going to show my mother this website so she can see that she is not alone. Right now, I thinks she feels like she is the only one in the world that could possibly have this crazy thing happen to her stomach. Up until this happened to her, we had never heard of such a thing….for someone’s stomach to just stop working!! I hope this website will give her some much needed HOPE! Lately her spirits are down and she’s been talking about wanting to just come home and stopping all treatment (including her dialysis) and starting hospice care….but as I said, she feels hopeless and like nobody could possibly live this way.
Thank-you for your inspiring story!! May God bless you!
Kirby says...
For drainage around tube sites (it is common but can be very irritating to the skin) – I suggest a dressing. They have super cute ones that might make your mother smile. Maybe order a few for her and gift them over to her to try out. They are also washable so they are re-usable. Again, they are so cute! I always give in to children patterns; no one sees it anyway so you might as well be fun with it! My favorite ones are found at these sites:
http://www.tubiewhoobies.com/#!g-tube-pads (these fit around the tube and then snap to stay snug and will absorb all the drainage)
http://www.mybuttonbuddies.com/ (you can go for skin colored ones but those aren’t any fun! and these use velcro I think. I prefer snaps but sometimes they are hard to snap…)
Also – here is a video for her. She is very much, not alone 🙂 These are only a “few” of my friends who have some sort of GI disorder, some due to other problems like autoimmune diseases, and some simply have “just” the GI disorder. They are of all ages! We come together and through our support of each other, we are stronger!
DTP (GP/CIP/MITO) Friends from Natiebar on Vimeo.
AND
Beth says...
Thanks so much for posting such a positive explanation of what you are dealing with. My mother who is 88 has been dealing with malnutrition for the last two years. When I was young she had a bleeding ulcer and at that time they removed the area that had the ulcer. So she has been dealing with the dumping syndrome of that for years. Just for the last 2’years she started losing weight. Going from 92 lbs down to 74 ish before they did the nasal tube (which she hated) and then the j-tube on which she gained all the weight back, but it was so horrible to have on with all the leaking so she had them take it out. She then dropped to 68.5 lbs, we got her admitted yesterday to the hospital, they finally got TPN started tonight and say she will be on it for 24 hours and then they will send her home with it. Of course Medicare is going to be dealing with this. Thankfully we have an appointment at the mayo clinic on Monday. But she will have to travel with this whole new contraption. I hope it works out!